Does clinical research account for diversity in deploying digital health technologies?
Explore the pivotal role and challenges of Digital Health Technologies in ensuring equitable and inclusive clinical research practices.
Embarking on a journey through the intricate landscape of digital health technologies (DHTs) and their role in clinical research, it becomes evident that these technologies harbour the potential to reshape and enhance the inclusivity and equity of research practices. The pivotal role of DHTs in clinical research is underscored by their capacity to broaden access, especially by enabling remote monitoring and thereby reducing the patient burden, which is crucial in ensuring that life-enhancing and life-saving treatments are accessible to the wider public.
However, an examination of the existing literature and studies reveals a notable gap in the representation of various social determinants of health (SDoH) within DHT-enabled clinical research. SDoH, which encompass conditions related to the environments where people are born, live, learn, work, and age, have a profound impact on health outcomes and quality of life. The inclusion and thorough reporting of groups adversely affected by SDoH in clinical research could potentially bridge disparities that limit the generalization of diagnostic or therapeutic modalities.
DHTs, which include a myriad of physical and software-based tools such as wearable sensors, artificial intelligence, and machine learning algorithms, ostensibly enhance access to clinical research by mitigating the need for cumbersome clinical visits, which are a staple of traditional monitoring during clinical trials. For instance, cardiac arrhythmias can now be monitored continuously and remotely, thereby not only improving access to clinical research but also enhancing the quality and granularity of data, which in turn, augments insights into disease treatment.
The representation of SDoH domains among study cohorts is often underreported, which curtails confidence regarding whether the results of studies are generalizable to the broader population. This is particularly pivotal in the context of DHT-enabled clinical research, given the intention to utilize them to amplify trial accessibility. The disparities in health outcomes and access to advancements in medical technology and care, particularly among socioeconomically disadvantaged groups, underscore the imperative to ensure that underrepresented groups are able to contribute to development programs.
A comprehensive evaluation of 126 DHT-enabled clinical research publications revealed a notable scarcity in the reporting of participant SDoH data. For instance, while Sex, Race, and Education were most frequently reported (in 94.4%, 27.8%, and 20.6% of publications, respectively), the remaining 8 domains were reported in fewer than 10% of publications. This lack of standardised reporting and systematic documentation of SDoH in clinical research publications presents a tangible opportunity to enhance reporting on the representation of SDoH among participants, thereby fostering equitable and inclusive research progress through DHT-enabled clinical studies.
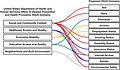
Moreover, the study proposed a framework wherein 11 SDoH domains could be captured and subsequently reported in future studies, utilizing medical codes that map to each of the proposed SDoH domains. This resource is suggested to illuminate that existing infrastructure could be leveraged to capture SDoH data, thereby paving the way for increased reporting and encouraging equitable and inclusive research progress through DHT-enabled clinical studies.
In light of these findings, it becomes paramount to advocate for the increased reporting of SDoH data in clinical research that deploys DHTs. The development and implementation of a standardised reporting framework for SDoH in clinical research publications, coupled with the systematic documentation of SDoH, could potentially foster transparency towards disparities that may be mitigated or perpetuated by the use of such technologies.